The Science Behind Being a Human Pin Cushion
Jennifer Valerio2022-10-11T17:07:14+00:00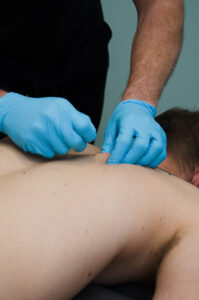 Here at IP, dry needling is a frequently utilized treatment that contributes to a comprehensive, personalized treatment plan. There are some great benefits to dry needling that include, but are not limited to, quick pain relief, improving range of motion, achieving a quicker path to recovery and more! Dry needling is also called trigger point dry needling or myofascial trigger point dry needling. The word “myofascial” is made up of the roots “myo” (which refers to muscle) and “fascia” (which refers to the tissue that connects muscle).
Here at IP, dry needling is a frequently utilized treatment that contributes to a comprehensive, personalized treatment plan. There are some great benefits to dry needling that include, but are not limited to, quick pain relief, improving range of motion, achieving a quicker path to recovery and more! Dry needling is also called trigger point dry needling or myofascial trigger point dry needling. The word “myofascial” is made up of the roots “myo” (which refers to muscle) and “fascia” (which refers to the tissue that connects muscle).
Injections into the myofascial trigger points were first proposed by medical doctors Janet Travell and David Simons in the early 1940’s. Travell discovered that certain nerves and neural hyperactivity were linked to pain in tender parts of the muscle and fascia. She and Dr. Simon carefully identified most of the trigger points located in the human body. They injected various substances including corticosteroids, painkillers, saline, etc. into the trigger points. That was the beginning of how modern dry needling was established. Dr. Travell was well respected and actually became President John F. Kennedy’s White House physician!
Seeing how the process originally used liquid to treat the trigger points, it’s a wonder why the procedure itself would be coined as “dry” needling. However, after Dr. Travell’s initial discovery, a study done by a Czech physician, Dr. Karel Lewit, found that the needling is what made the treatments effective, far more than the substances that were injected into the muscles. Further research proved that dry needling is more effective and not as invasive as “wet” needling, though it was only in 1976 when the procedure became a recognized practice in the healthcare industry. It was Dr. Chan Gunn who further developed the concept of dry needling. He researched the technique of Intramuscular Stimulation (IMS). IMS is a technique for the treatment of myofascial pain based on a comprehensive diagnostic that identifies the cause of the pain due to disease or dysfunction in the nervous system. It specifically identifies the nerve root as the generator of the anatomy, so it is referred to as a radiculo-neuropathic model.
Muscles can develop knotted areas called trigger points. These trigger points are very sensitive and can be painful when touched. Our PTs will insert needles through the skin into trigger points. Those needles are used as a reset for the golgi tendon organ (GTO) to stimulate the tissue, not to inject medication.
Pain affects how your body moves. Dry needling changes the way the brain and muscles talk to each other to help your system return to normal function.
You may experience different sensations when being needled. Muscle soreness, aching and an elicited muscle twitch when a needle is inserted are considered good signs of effective needling. The needles may be placed deeply, for various amounts of time, depending on what type of pain is being treated and pathology. Shorter periods of time would mean that the needle would stay in the muscle for seconds, while longer periods could mean 10 to 15 minutes.
Now you have a basis of where dry needling comes from and why we use it. Never hesitate to ask us more, we are all happy to explain why we love dry needling!

 surgery [surgery is a top one] but PRP, marathon/military training or even activities of daily living are included. Prehab differs from rehab in that it is a proactive plan designed to prepare you for whatever life brings at you next. Here at IP, you know we love pumpin’ prevention to help patients optimize their potential!
surgery [surgery is a top one] but PRP, marathon/military training or even activities of daily living are included. Prehab differs from rehab in that it is a proactive plan designed to prepare you for whatever life brings at you next. Here at IP, you know we love pumpin’ prevention to help patients optimize their potential!